When it involves drug pricing, each the Trump and Biden-Harris administrations have had some very modest successes.
As director of the Health Outcomes, Policy and Evidence Synthesis Group on the University of Connecticut School of Pharmacy, I teach and study on the ethics of prescription drug pricing and the complexity of drug pricing on the national level.
If you look closely on the successes of the presidential candidates on a spread of drug pricing policies, you will note that these advances have continued under each administration. However, neither the Trump administration nor the Biden-Harris administration have done anything to actually lower drug prices for nearly all of Americans.
35 dollars insulin
Insulin is a necessity for patients with diabetes. However, from January 2014 to April 2019, the common price per unit increased from 0.22 to 0.34 US dollars before declining barely to $0.29 per unit by July 2023. Because dosing relies on weight, insulin costs for a 154-pound person would have increased from $231 to $357 monthly from 2014 to 2019, after which decreased to $305 monthly by 2023. Price increases have caused some patients to take their medications for longer periods of time, taking lower than the dose they need for good blood sugar control. One study estimated that over 25% of patients In an urban diabetes center, patients were using too little insulin.
In July 2020, the Trump administration issued a $35 cap on insulin Copayments were introduced by executive order. In fact, participating Medicare Part D programs were forced to cap the worth of only one insulin product of every type at $35. For example, if six short-acting insulin products were on an insurance plan's list of approved drugs, the insurer had to supply one vial and one pen form for $35.
These price changes didn’t come into effect during Trump’s presidency. Until 2022, only about 800,000 people – or around 11% of the over 7.4 million people within the US who use insulin to manage their blood sugar – have lowered their prices.
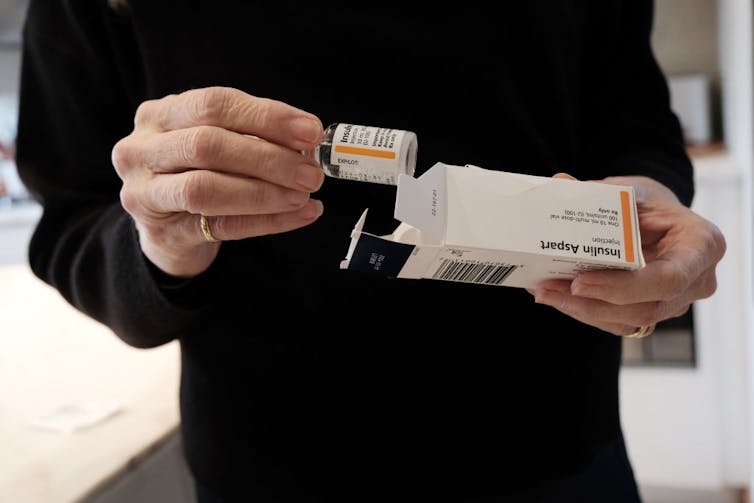
Spencer Platt/Getty Images
In August 2022, the Biden-Harris administration signed the Inflation Reduction Act This maintained the $35 cap on insulin with the identical terms, but made this system mandatory for all Medicare Part D and Medicare Part B members, increasing the number of people that may gain advantage from cheaper insulin to three.3 million.
That still doesn’t help most diabetics. If you don't have Medicare, the $35 discount doesn't apply to you. Also, under these policies, drug corporations aren't answerable for reducing insulin costs; medical insurance corporations are answerable for reducing copayments. The costs may very well be passed on to beneficiaries in future Medicare premiums.
Importing Canadian medicines
Americans pay almost 2.6 times more for pharmaceuticals than people in other high-income countries. One way regulators have tried to bring down prices is to easily import drugs at the costs that pharmaceutical corporations charge in those countries, quite than the costs charged to U.S. consumers.
In July 2019, the Trump administration proposed Importing medicines from Canada to share the lower drug costs for Canadians with American consumers. He signed an executive order allowing the Food and Drug Administration to set the foundations under which states could import the drugs. When President Joe Biden took office, he left the manager order in place and the legislative process continued.

Jeff Haynes/AFP via Getty Images
No state under the Trump or Biden-Harris administrations has been capable of successfully import a Canadian drug. However, in January 2024, the Food and Drug Administration approved Florida’s plan to import Canadian medicinesthe primary state to receive the green light. Colorado, New Hampshire, New Mexico and Texas have submitted applications through September 2024.
Unfortunately, it’s unlikely that Canada would allow the shipping of its pharmaceuticals in large quantities to American consumers, not without Introduction of high tariffs as a deterrent. This is because drug manufacturers could limit their supplies to Canada and cause shortages if drugs are shifted to the US. Manufacturers might also be less willing to barter lower prices for Canadians if doing so hurts US profits.
Negotiations with the pharmaceutical industry
Whether it's pharmaceuticals or cars, buyers and sellers must agree on a price for a sale to achieve success. If the possible buyer isn't willing to interrupt off negotiations, you won't get the vendor's best price. One reason drug prices are higher within the U.S. than in other countries is because the federal government isn't a talented negotiator.
Negotiations that result in significant price reductions for medicines often result from the drug manufacturer losing access to patients on a selected health plan or landing in the next drug tier that significantly increases the patient's copayment. However, if the client rejects the vendor's final offer, its members or residents lose access to those drugs. While large private health insurers and pharmacy profit managers can negotiate drug prices directly with drug manufacturers, often leading to significant savings, Medicare was prevented from doing so until recently by federal law.
In May 2018, the Trump administration published a so-called Blueprint for lowering prescription drug prices This included negotiations with the pharmaceutical industry over prescription drug prices under Medicare, but this plan was not implemented during his term.
In August 2022, under the Biden-Harris administration, the Inflation Reduction Act enables price negotiations and indicated the number of medicine that may very well be negotiated in a 12 months.
The first negotiation between Medicare and the pharmaceutical industry took place in the summertime of 2024 and resulted in a discount in the fee of 10 Medicare Part D drugs, including the blood thinner Xarelto and the drugs Farxiga and Jardiance, which treat type 2 diabetes, heart failure and kidney disease. The resulting savings of $1.5 billion might be prolonged to the roughly 8.8 million Medicare Part D patients who take these drugs in 2026. Prices for these drugs are still twice as much as in 4 other industrialized countries.
In 2027, prices for 15 more Medicare Part D drugs might be subject to cost negotiation. After that, drug negotiations could also include Medicare Part D drugs that you simply pick up at your pharmacy and Medicare Part B drugs which are distributed or obtained at your doctor's office.
Another aspect of the Inflation Reduction Act is the limitation Expenses of USD 2,000However, this may not come into force until 2025 and any costs above the cap will simply be passed on to taxpayers.
Continuing progress
When assessing complex issues corresponding to drug pricing, it is commonly difficult to attribute policy successes to at least one administration or one other. Ideas were initiated throughout the Trump administration that were only implemented and expanded under the Biden-Harris administration.
For example, the Medicare price negotiations proposed in a Trump administration “plan” were signed into law by President Biden, however the fruits of this policy is not going to be seen until the following administration. And no matter who you credit for this success, only a portion of Medicare beneficiaries will see relief from high drug prices because of this.
To really reduce the fee of pharmaceuticals, one would need to determine the utmost price that the country is willing to pay for services corresponding to Costs per quality-adjusted life 12 months at federal, state and personal payer levels and the willingness to interrupt off negotiations if the worth exceeds this level. However, this may not be a panacea, especially for patients with rare and really rare diseasesand would must be adapted over time to avoid bankruptcy of the industry.
image credit : theconversation.com


















Leave a Reply